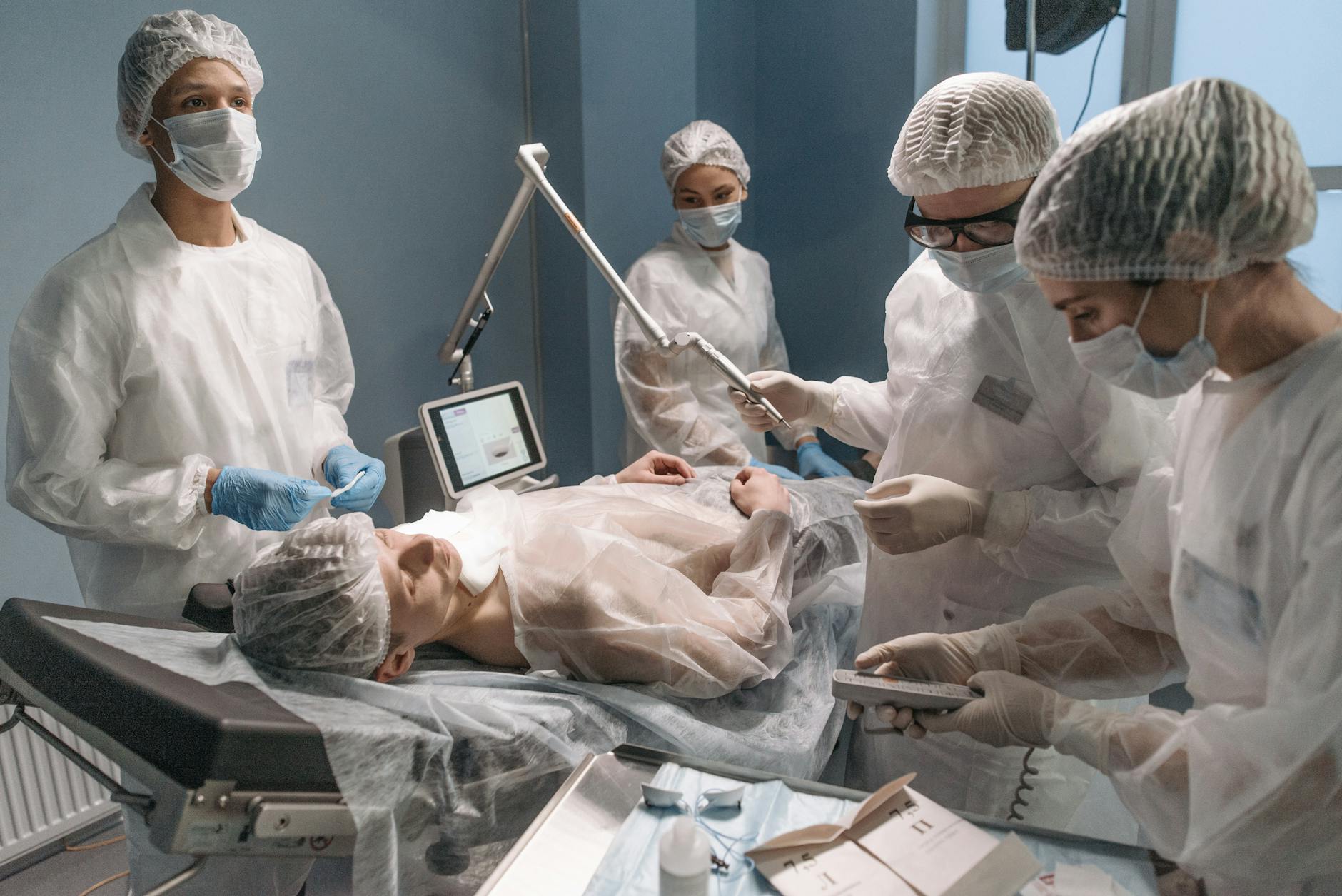
MBOT, developed by Monogram Orthopaedics, represents a new category in surgical robotics””one that prioritizes accessibility, precision, and data-driven intelligence in ways that mirror how Google transformed information access. The comparison to Google is not about market dominance but about architectural philosophy: just as Google built a platform that learns from every search to improve subsequent results, MBOT is designed to collect surgical data from every procedure and feed it back into an increasingly intelligent system. This closed-loop approach to surgical automation marks a departure from legacy robotic systems that function more like expensive surgical GPS units than true learning platforms. The MBOT system specifically targets total knee arthroplasty, a procedure performed over 700,000 times annually in the United States alone.
Unlike larger competitors such as Intuitive Surgical’s da Vinci or Stryker’s Mako, MBOT was engineered from the ground up to be compact, affordable, and capable of autonomous bone preparation. In early clinical applications, surgeons have reported bone cuts within 1 degree of planned positioning””a level of precision that would be nearly impossible to achieve consistently by hand. The system’s small footprint also means it can fit into ambulatory surgery centers rather than requiring the infrastructure of a major hospital operating room. This article examines what makes MBOT’s approach distinct, how its autonomous capabilities compare to surgeon-controlled alternatives, the technical specifications driving its performance, and the regulatory and adoption hurdles that remain. We will also address limitations that hospitals and surgeons should understand before considering implementation.
Table of Contents
- Why Is MBOT Being Called the Google of Surgical Automation?
- Technical Specifications and Autonomous Capabilities
- How MBOT Compares to Established Surgical Robotics Platforms
- Regulatory Pathway and Clinical Validation Status
- Training Requirements and Implementation Considerations
- Economic Impact on Ambulatory Surgery Center Viability
- Future Development and Platform Expansion Potential
- Conclusion
Why Is MBOT Being Called the Google of Surgical Automation?
The “google of surgical automation” label stems from MBOT’s foundational design principle: building a data platform first and a robot second. Monogram Orthopaedics developed proprietary software called mVision that processes preoperative CT scans to generate patient-specific surgical plans. These plans are not static; the system is architected to aggregate anonymized outcome data across all procedures, creating a feedback loop that refines planning algorithms over time. This mirrors Google’s approach of using user data to continuously improve search relevance. Traditional surgical robots operate more like sophisticated power tools””they enhance a surgeon’s mechanical capability but do not fundamentally learn or adapt. MBOT’s autonomous execution capability changes this equation.
During the bone preparation phase, the robot can perform cuts without continuous surgeon manipulation, using real-time sensor feedback to maintain sub-millimeter accuracy. The surgeon retains override authority and makes all strategic decisions, but the actual cutting becomes a machine-controlled process informed by the collective intelligence of the platform. However, this comparison has limits worth noting. Google’s value compounds with scale because more searches mean better algorithms for everyone. MBOT’s learning loop depends on surgical volume and outcome tracking that has not yet reached the scale needed to prove this network effect in practice. The company went public via SPAC in 2023 with a market capitalization around $130 million””significant for a medical device startup but modest compared to the billions commanded by established surgical robotics players. The Google comparison is aspirational as much as descriptive.

Technical Specifications and Autonomous Capabilities
MBOT’s hardware distinguishes itself through miniaturization. The robotic arm weighs approximately 25 pounds and mounts directly to the operating table, eliminating the need for a separate cart or dedicated floor space. This contrasts sharply with systems like Mako, which require a large mobile platform and significantly more operating room real estate. For ambulatory surgery centers operating in spaces under 2,000 square feet, this difference is not trivial””it can determine whether robotic surgery is physically feasible. The autonomous bone cutting function uses a six-degree-of-freedom arm with force-sensing capabilities that allow it to detect and compensate for bone density variations in real time. Preoperative CT scans are processed to create a three-dimensional bone model, and the mVision software generates a cutting plan optimized for the specific implant being used.
During surgery, the robot executes planar cuts for femoral and tibial preparation with reported accuracy within 1 degree of the planned angles. Traditional manual technique typically achieves 3-5 degree accuracy in the best hands. The limitation here involves the current scope of autonomy. MBOT handles bone preparation but not soft tissue work, implant insertion, or any of the judgment-intensive steps that determine overall surgical success. A perfectly cut bone surface means little if ligament balancing is poor or if the implant is seated incorrectly. Surgeons considering this technology should understand that MBOT automates perhaps 15-20 minutes of a 90-minute procedure, albeit a critical portion where precision matters most.
How MBOT Compares to Established Surgical Robotics Platforms
The surgical robotics market is dominated by players with decades of clinical history. Intuitive Surgical’s da Vinci system has facilitated over 10 million procedures. Stryker acquired Mako Surgical in 2013 for $1.65 billion and has since installed thousands of systems worldwide. Zimmer Biomet’s ROSA platform and Smith+Nephew’s CORI system represent additional entrenched competition. MBOT enters this field as a small company with limited clinical data challenging giants with established surgeon relationships and proven track records. Where MBOT differs is in the economic model.
A Mako system costs approximately $1 million to $1.5 million, with additional per-procedure costs for disposables and software fees that can exceed $1,500 per case. Monogram has indicated pricing targets significantly below these figures, though exact commercial pricing remains subject to negotiation. For independent orthopedic practices and surgery centers operating on thin margins, this cost differential could make robotic capability financially viable for the first time. The tradeoff involves ecosystem maturity. Mako has hundreds of peer-reviewed studies validating its outcomes. MBOT has early feasibility data and cadaver studies but lacks the long-term follow-up that demonstrates implant survivorship and patient satisfaction over 10+ years. Surgeons with existing robotic experience on competitor platforms face a learning curve when switching, and the referral networks built around established systems represent switching costs that pure technical specification comparisons fail to capture.
Regulatory Pathway and Clinical Validation Status
MBOT received FDA 510(k) clearance for its robotic system, establishing regulatory permission to market the device in the United States. This clearance came through the substantial equivalence pathway, comparing MBOT to predicate devices already on the market. The FDA review process for surgical robots does not require clinical trials demonstrating improved patient outcomes””only that the device is as safe and effective as existing cleared products. This is an important distinction that surgeons and hospital administrators sometimes misunderstand. The clinical evidence base for MBOT remains early-stage.
The company has published results from cadaveric studies demonstrating cutting accuracy and has conducted first-in-human procedures under investigational protocols. Long-term outcome data comparing MBOT-assisted procedures to manual techniques or competitor robots does not yet exist. This is normal for new surgical technology””data accumulates over years of commercial use””but it does mean early adopters are relying on engineering specifications rather than proven clinical track records. For surgeons evaluating whether to wait or adopt early, the calculus depends on risk tolerance and patient volume. High-volume joint replacement specialists may find value in participating during the technology’s maturation, contributing to the evidence base while potentially improving their own outcomes through enhanced precision. Low-volume surgeons without strong support infrastructure for troubleshooting new technology may benefit from waiting until the system has more field experience and the inevitable early software refinements have been implemented.
Training Requirements and Implementation Considerations
Adopting any surgical robot requires surgeon training, operating room staff education, and workflow redesign. MBOT’s training program involves simulation, cadaveric practice, and proctored cases where an experienced user observes the adopting surgeon’s initial procedures. The learning curve appears shorter than for some competitor systems because the surgeon’s intraoperative role is more supervisory””the robot executes the precision-critical cutting rather than requiring the surgeon to manually guide a robotic arm. Operating room integration presents practical challenges. The mVision software requires preoperative CT scans, adding an imaging step that some practices may not currently include in their joint replacement workflow.
CT scans involve radiation exposure and cost, though the dose for extremity imaging is low by medical standards. Practices accustomed to radiograph-only preoperative planning will need to establish imaging protocols and patient education explaining why the additional scan is worthwhile. The compact footprint that makes MBOT attractive for ambulatory surgery centers also means certain infrastructure assumptions must hold. Reliable high-speed internet connectivity is necessary for software updates and potential remote support. Power supply stability matters more when a robot is mid-cut than when a surgeon is working manually. These are solvable issues but represent the kind of implementation details that differentiate successful adoption from frustrating experience.

Economic Impact on Ambulatory Surgery Center Viability
The shift of total knee arthroplasty to ambulatory surgery centers represents one of the significant trends in orthopedic care delivery. CMS removed total knee replacement from the inpatient-only list in 2020, allowing Medicare reimbursement for outpatient procedures. This policy change created economic incentive for ASCs to build joint replacement capability, but the capital cost of surgical robotics has been a barrier for smaller facilities.
MBOT’s design specifically targets this emerging market segment. A system that costs less than competitors, fits in smaller spaces, and does not require a dedicated robotic operating room could accelerate ASC adoption of robotic-assisted arthroplasty. If the technology delivers on accuracy promises while maintaining the cost structure Monogram has described, it could reshape the competitive dynamics between hospital outpatient departments and independent surgery centers.
Future Development and Platform Expansion Potential
Monogram has indicated intentions to expand beyond total knee arthroplasty to additional joint replacement procedures. Total hip arthroplasty represents an obvious adjacent market, though the surgical anatomy and workflow differ enough that meaningful development work would be required. Unicompartmental knee replacement, revision surgery, and potentially shoulder arthroplasty could follow, though each application requires specific engineering adaptation and separate regulatory clearance.
The data platform aspect of MBOT’s architecture creates interesting possibilities beyond execution accuracy. If the system accumulates sufficient procedure data with outcome tracking, it could potentially generate insights about optimal implant positioning, patient selection, and surgical technique that improve care system-wide. This is the genuine promise behind the Google comparison””not just making one robot precise, but using aggregated intelligence to elevate the entire field. Whether Monogram achieves this potential depends on commercial adoption, data infrastructure investment, and the willingness of surgeons to share outcome information in ways that have historically faced resistance.
Conclusion
MBOT represents a genuine architectural innovation in surgical robotics: a compact, relatively affordable system designed with autonomous execution capability and an underlying data platform that could improve over time. For ambulatory surgery centers and independent orthopedic practices, it offers a potential path to robotic capability that larger systems have priced out of reach.
The precision specifications for bone cutting are impressive and address a real clinical need in joint replacement surgery. The technology remains early in its commercial deployment, with limited clinical outcome data and the inevitable uncertainties of adopting any new surgical system. Surgeons and healthcare administrators should evaluate MBOT on its current demonstrated capabilities rather than its aspirational potential, while recognizing that the design philosophy””learning from every procedure to improve the next one””represents the direction surgical automation is likely to evolve regardless of which company leads that transformation.